Cardiovascular Simulation Lab features 3D Printing to Improve Heart Surgery Techniques
Published: Jan 11, 2021By Tampa General Hospital
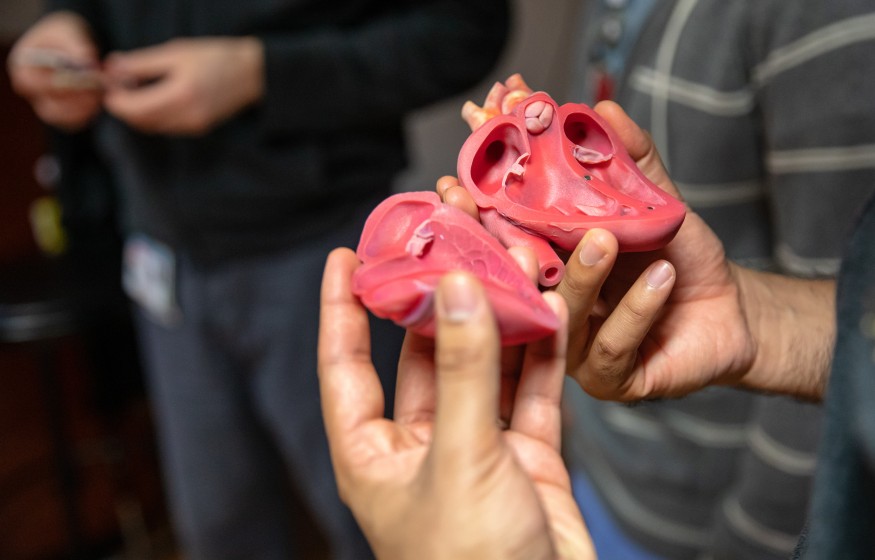
There’s something dramatic and innovative occurring as Dr. Fadi Matar guides a catheter into a heart at Tampa General Hospital and carefully places a tiny plug to repair a hole. What’s innovative is the heart itself – it’s made of plastic and was created in a highly sophisticated 3D printer.
This gray plastic heart is an example of clinical 3D printing, which means this is not just a plastic model but a replica of a living heart from a real patient – accurate in size and shape to within one hundredth of an inch. The accuracy means surgeons can use replicas of hearts to visualize and practice operations in ways that were impossible just a few years ago.
Dr. Matar, for example, was practicing and evaluating an operation that would call for him to insert a catheter through a major vein and into the patient’s right atrium, and then into the left atrium. He would then place a surgical plug into a hole near the patient’s mitral valve. The plastic heart was helping Dr. Matar as he evaluated different aspects of the operation, including which sized surgical plug would be best.
Dr. Matar, who is Associate Professor and Interventional Cardiologist in the USF Health Morsani College of Medicine, specializes in coronary and structural interventional cardiology, and his research interests includes the use of 3D printing for the management of structural heart intervention.
Tampa General Hospital and the USF Health Morsani College of Medicine have become the first in Florida to establish a 3D Cardiovascular Simulation (3D-CVS) laboratory, which is responding to the need for more advanced assessment tools and technologies to treat more complex cardiovascular diseases.
At the 3D-CVS laboratory, complex structural procedures are simulated and planned for by placing printed cardiac models in specially designed cradles, mimicking the heart’s position in the chest. Interventional catheters are then introduced through modeled vessels to deliver the specific devices as they would be during a real procedure. Such models, when coupled with circulatory simulations, can give valuable hemodynamic information on the performance of the implanted device before actually performing the procedure on that patient.
The use of 3D printers not only helps surgeons decide when to operate, it helps them decide when not to. This allows surgeons and patients to make the best-informed choices possible to avoid unnecessary surgeries.
“We’ve been able to save lives, cut operating times by hours and make things more efficient and safer,” said Summer Decker, PhD, Associate Professor, Vice Chair for Research, and Director of 3D Clinical Applications for the Department of Radiology in the USF Health Morsani College of Medicine.
