Rewiring the Body’s Plumbing: Tampa General Hospital and USF Health’s Dr. Nicholas Panetta Changes Lives of Lymphedema Patients Through Innovative Surgical Techniques
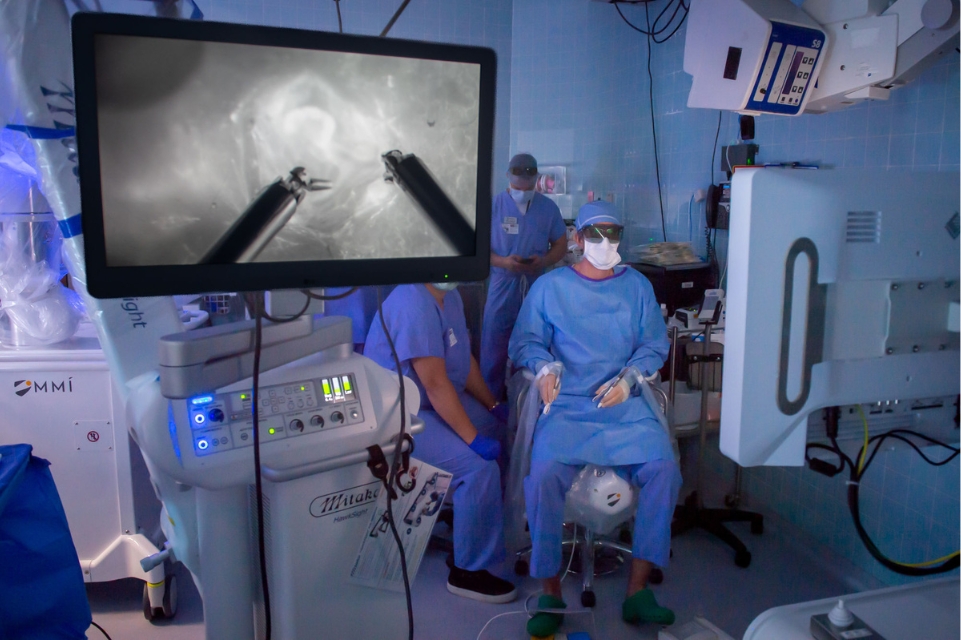
One of the few surgeons worldwide licensed to use the Symani Surgical System, this advanced robotic microsurgery system helps prevent damage or restore function to the lymphatic system.
For many patients recovering from cancer and other conditions, the end of treatment does not mean the end of medical challenges. Lymphedema is a frustrating and often misunderstood condition. The chronic disorder causes painful swelling in the arms or legs when the body’s lymphatic system stops working properly.
Dr. Nicholas Panetta, chief of the Plastic Surgery Institute at Tampa General Hospital (TGH) and chair of the USF Health Morsani College of Medicine Department of Plastic Surgery, is among a few surgeons worldwide trained to use a novel approach for this condition: a highly specialized robotic platform — the Symani Surgical System — to perform microscopic procedures that restore lymphatic drainage. The technology is opening a new chapter for patients who once had few options beyond cumbersome lifelong symptom management.
A Hidden Burden
The lymphatic system is part of the body’s immune and fluid‑drainage network. Thin channels carry lymph fluid through the body and return it to the bloodstream. But when lymph nodes or vessels are damaged or removed, the system can become blocked, causing fluid buildup, painful swelling and other complications.
The result is lymphedema.
“Think of it as a plumbing problem,” Dr. Panetta said. “Fluid keeps coming into the arm or leg, but because the normal drainage pathways have been disrupted, it can’t get out.”
The numbers are significant. Up to 250 million people worldwide have lymphedema, with an estimated 10 million living with the condition in the United States, more than HIV, Parkinson’s disease, multiple sclerosis, muscular dystrophy and ALS combined.
Learn more about the incidence of lymphedema.
The condition can profoundly affect daily life. Arms or legs may become swollen, painful and difficult to move. Patients often must wear tight compression garments every day, undergo specialized massage therapy or use pumps to move fluid out of the limb. In severe cases, repeated infections called cellulitis can require hospitalization and intravenous antibiotics.
“It can dominate people’s lives,” Dr. Panetta noted. “Managing lymphedema can become a full‑time job.”
From Symptom Control to System Repair
For decades, treatment focused mainly on managing symptoms rather than remedying the underlying problem, which worsens over time. Compression sleeves and physical therapy can help push fluid out of swollen tissues, but they do not restore the underlying damage. Microsurgery aims to change that.
Using a technique called lymphatic‑venous bypass, surgeons connect tiny lymphatic vessels directly to nearby veins. The new pathway allows lymph fluid to drain back into the bloodstream, bypassing the damaged lymph channels.
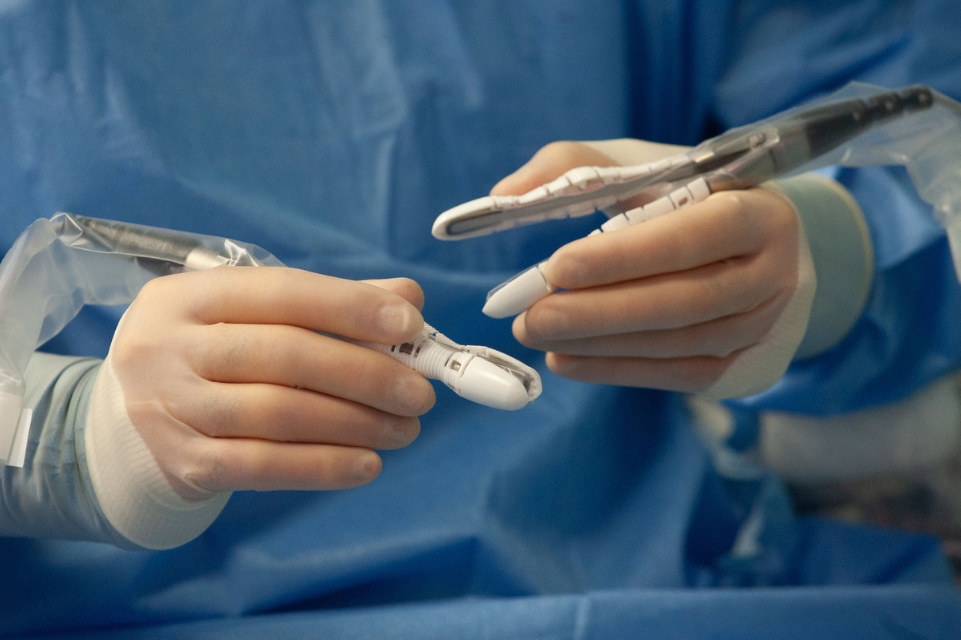
The challenge is scale. Most lymphatic vessels are less than 1 millimeter in diameter — about the size of a sharpened pencil tip. Extraordinary precision is required when operating on structures that small.
A Robot Built for Microscopic Surgery
Robotic surgery is addressing the issue. Unlike larger surgical robots designed to work inside the body cavity, the Symani Surgical System was built specifically for open microsurgery.
The robot eliminates natural hand tremor and dramatically scales down a surgeon’s movements. A motion of 1 centimeter by the surgeon’s hand can be reduced to just a fraction of a millimeter at the surgical site.
That precision makes it possible to stitch together tiny vessels and keep them open — what surgeons call patency — so fluid can flow properly. “It allows us to place sutures with an accuracy that’s never really been possible before,” Panetta said.
TGH acquired the technology through a collaboration between TGH’s cancer program, USF Health and the state of Florida. Worldwide, only a few hundred surgeons perform these procedures.
Better Outcomes — Especially When Caught Early
Success in lymphedema treatment is influenced by timing.
When surgeons intervene early — before the disease begins or progresses — they are more likely to restore normal function. Patients may eventually stop wearing compression garments and return to normal activities.
Even in moderate cases, surgery can significantly reduce swelling — often by 30 to 40 percent — and prevent the condition from worsening. Many patients experience relief from the heaviness, tightness and limited mobility that define daily life with lymphedema.
“Stopping the disease from progressing is a huge win,” Dr. Panetta said.
A Patient’s Story
For TGH patient Monica Boney, the condition developed far from home.
While serving in the U.S. Army in Afghanistan, Monica suffered a spider bite that led to a severe infection that damaged her lymphatic system, leaving her with stage 2 lymphedema in her leg.
After seeking care for more than two decades to manage symptoms, she underwent lymphatic reconstruction surgery at TGH. The procedure involved only tiny incisions — about 1 centimeter long — and the swelling was immediately improved. Recovery was swift. Within weeks, Monica returned to an active lifestyle and completed a 75‑mile cycling event supporting the Wounded Warrior Project.
Stories like hers illustrate what modern microsurgery can offer patients who once had little hope of improvement.
A Multidisciplinary Approach
TGH’s dedicated lymphedema clinic is rooted in academic medicine, employing a team approach to identify new treatment options and manage the condition. Surgeons work alongside nurses, therapists, imaging specialists and nutrition experts.
Patients undergo a comprehensive evaluation, including limb measurements and specialized lymphatic imaging, before treatment decisions are made.
Lifestyle factors such as weight management are also addressed, because excess body weight can worsen lymphedema by increasing pressure in nearby veins. The TGH team’s goal is to intervene as early as possible — sometimes even preventing the condition altogether.
Dr. Panetta believes robotic microsurgery could dramatically expand access to these procedures in the future. “The robot helps democratize microsurgery,” he said. “It gives us a tool to train more surgeons and get these treatments to more patients.”
For people living with lymphedema — or at risk of developing it — that could mean a future where the condition no longer defines their lives. And for many patients, it represents something simple but powerful: the chance to move freely again.
